In my blog last week, I consciously decided to avoid the Covid-19 topic. The situation was evolving day to day and I asked myself what useful insights or comments I could possibly have.
Just 11 days ago, the cancellation of HIMSS20 conference was announced. Many of us were hoping for this as we worried about being in a convention center with 45,000 people from not just around the country but around the world. With the cancellations of major sports, Broadway, closure of Disney, limits on the size of large gatherings, and school closings, the times have changed drastically in a matter of days.
We are being encouraged to practice “social distancing”. People who can are working from home.
But hospitals remain open for business as they must. Our nurses and doctors are on the front lines. IT teams and all the hospital staff who support the clinicians are doing what is necessary to ensure that they can deliver care.
While all healthcare organizations have emergency preparedness plans in place for a variety of incidents, this is uncharted territory that tests the limits of those plans. There will be much to learn and share when we get to the other side of it. But in the spirit of we’re all in this together and the culture of sharing best practices we have in healthcare, here are a few links that might be of value in the days ahead.
UW Medicine CIO’s advice: Prepping IT systems for COVID-19 – by Eric J. Neil published in Health IT News, March 12. UW Medicine was one of the first health systems on the front lines of the pandemic in the U.S. Their insight and advice are invaluable to IT leaders around the country.
While you may question the value of Twitter, it is yet another forum where lessons are being shared from the front lines. Dr. Kira Newman has worked in the ICU in Seattle the past week and posted a 10 part thread:
In one part Dr. Newman provided the link to their Covid-19 Resource Site for other hospitals to use.
17 Coronavirus (Covid-19) Actions for Healthcare CIOs – by John Lynn in Healthcare IT Today, March 11. John is continuing to collect info from IT leaders and will share as he does.
Healthcare IT News is maintaining a list of trusted resources that can be found here: Key resources to keep track of the coronavirus pandemic.
Most of my readers probably work in healthcare organizations and fully understand the magnitude of this pandemic. For those of you who don’t and need some convincing, remember that science and math do matter. Here are two of the best articles I’ve seen:
Why Outbreaks Like Coronavirus Spread Exponentially and How to Flatten the Curve – by Harry Stevens in the Washington Post, March 14.
Coronavirus: Why You Must Act Now – Politicians, Community Leaders and Business Leaders: What Should You Do and When? – Tomas Pueyo, first written March 10 and updated on March 13. The author closed with this message: “This is probably the one time in the last decade that sharing an article might save lives. They need to understand this to avert a catastrophe. The moment to act is now.” So, I share with all of you.
And if working from home is new to you, here’s a good resource to check out:
Work in the time of Corona – a blog by Alice Goldfuss on March 11th.
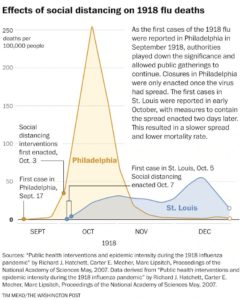
My paternal grandfather died in the 1918 flu pandemic. He was young but married with three small children. My father and uncle were sent to an orphanage and my grandmother and aunt went to live with friends. Yes, it’s not 1918. Healthcare has advanced significantly. But we are an even more global and mobile society. The most important lesson from 1918 is the impact of social distancing which is shown in this graph:
In closing, I want to express a huge thank you to all who work in healthcare. The strain on our healthcare system is real. The stress on our healthcare workers is real. Let’s all do our part to #SlowTheSpread and #FlattenTheCurve.